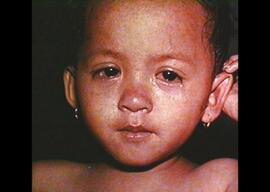
 We’ve been hearing a lot about measles in Oregon in the past couple of weeks. There has been a lot of discussion online (and a lot of misinformation). What is it? Is it really that bad? Why is it spreading all of the sudden? Measles is caused by a virus that’s spreads through respiratory droplets. Those are the little particles that are thrown into the air when someone coughs and sneezes. At first a person with measles just looks like they have a cold. Early symptoms are cough, stuffy nose, and red eyes. Eventually, the person will develop a high fever (up to 105 or 106), light sensitivity, and a red rash that starts at the hairline and moves down the body. People with measles are usually sick for about 3 weeks. The virus is very contagious, infecting about 90% of susceptible (not immune) people who are exposed to it. Viral particles can remain in the air and infectious for up to 2 hours after the person who produced them has left the area, so you can be exposed to measles without ever laying eyes on the person who exposed you. It is contagious for 4 days before the rash appears to 4 days after the rash appears, so someone with measles is shedding this very contagious illness before they even know they are sick with it. This is why there are so many potential exposure sites in and around the Portland and Vancouver area and why the disease continues to spread. For more information about measles and the vaccine, the CDC Pink Book has great information.
Complications of measles infection are common, occurring in 1 of every 3 people who gets sick with it. Complication rates are higher in kids under 5, adults over 20, pregnant women, and people with a weakened immune system. Complications include diarrhea, viral pneumonia and croup, eye scarring and blindness, kidney failure, low platelets, myocarditis (heart inflammation), myositis (muscle inflammation), and encephalitis (brain inflammation). The risk of eye scarring can be reduced with vitamin A supplementation, so people with measles are routinely given vitamin A. Otherwise, there is no treatment. The death rate from measles infection is 1-2/1000, usually from pneumonia, encephalitis, or myocarditis. The death rate decreased significantly throughout the 20th century but hasn’t really changed since the 90s. There is also a complication called subacute sclerosing panencephalitis (SSPE) which occurs in 1 in 10,000 people who get the measles about 7-10 years later. It causes gradual, progressive neurological deterioration with death usually occurring within 3 years. If caught early, symptom progression can be slowed (but not stopped) with antivirals for the rest of the person’s life. When someone recovers from measles, their immune system is basically reset. They have an increased risk of all infectious diseases, including an increased risk of dying of infectious disease, for years after measles infection until the immune system "relearns" all of the protection it lost. The measles vaccines were first licensed in 1963. There were initially two versions, a killed version and a live-attenuated (live virus that has been modified to make it not infectious) version. The killed version was taken off the market in 1967, and the current strain of the live-attenuated version has been in use since 1968. It is given as a 2 dose series with 95% of people developing immunity after 1 dose and 99% after 2 doses. Immunity from the vaccine is lifelong. The second dose was added in 1989, so some adults may not have gotten 2 doses. The measles vaccine was combined with mumps and rubella into the MMR vaccine in 1971. Since that time, over 500 million doses have been given worldwide. The type of immunity induced by the MMR vaccine (humoral immunity) is not fully effective until after 12 months of age. Infants get some immunity through the placenta from mom, but that usually wanes by about 6 months. In outbreak situations, after a known exposure, or if traveling to a measles-endemic area, an infant between 6 and 12 months can get an extra MMR dose before 12 months but will still need 2 doses after 12 months. The first dose is typically given at the 12 or 15 month check-up, and the second dose between 4 and 6 years old. The second dose can be given as early as 28 days after the first dose. More common adverse reactions to the vaccine include fever and rash (usually a red splotch around the vaccine site). About 1/4 of adult women who get the vaccine report joint pain afterward. This is from the rubella component of the vaccine. Low platelets occur in 1 out of 30,000-40,000 doses (just like you get low platelets with measles disease). No deaths have been reported from these low platelets. The Institute of Medicine and the American Academy of Pediatrics, both nongovernmental groups, have evaluated the MMR vaccine and its reported association with autism, and both concluded, after reviewing multiple studies including hundreds of thousands of participants, that there is no association. Additional information on the safety of the MMR vaccine can be found here, here, and here. Comments are closed.
|
About the blogA look at some topics in breastfeeding, medicine, and kids health. Archives
December 2019
Categories |
 RSS Feed
RSS Feed